When we think about the causes of climate change, the usual suspects often come to mind: coal-fired power plants, traffic-choked roads, industrial agriculture. Rarely do we picture hospitals.
Yet if global healthcare were a country, it would be one of the world’s top five greenhouse gas emitters. With healthcare responsible for about 5% of total global emissions. This puts it on par with some of the most polluting industries on earth.
The far-reaching consequences of climate change are increasingly recognised as the greatest threat to human health in the 21st century.
Rising temperatures and environmental disruption are already harming on human health. Indeed, this can be seen in the increase in heart and lung disease, the spread of infectious diseases carried by insects, heat-related illness, injuries from extreme weather events and worsening mental health. And then there are issues of disrupted access to clean water, food and shelter.
This reveals an uncomfortable truth: healthcare is both a protector of health and a contributor to one of its greatest threats.
Inside hospital emissions
One of the most surprising aspects of healthcare’s carbon footprint is where most of the emissions come from. While hospitals themselves use large amounts of energy, most emissions – up to 70% – actually arise from the healthcare supply chain itself.
This includes the manufacture, transport and disposal of pharmaceuticals, medical devices, reusable equipment and single-use items such as gloves, masks and syringes.
Modern medicine depends heavily on these products and every item carries its own hidden environmental cost. This means that the carbon footprint of healthcare is not just tied to buildings and electricity use, but to the entire global network required to deliver care.
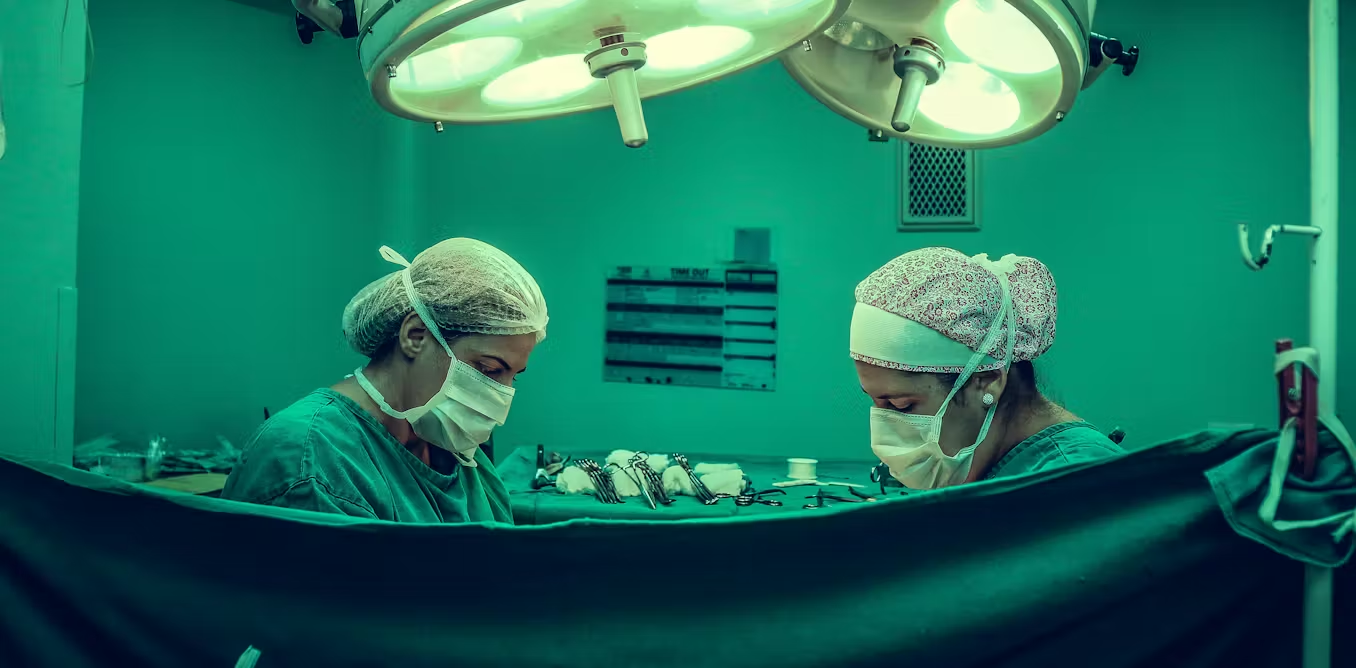
Canva/Holly Squire
Hospitals themselves are a major source, accounting for around 30% of healthcare-related emissions in high-income countries. With operating theatres three to six times more energy intensive than other hospital areas.
Individual surgical procedures can also have significant carbon footprints. For example, a heart bypass operation has been estimated to be roughly equivalent to driving 1,700 miles in a petrol car. And even a tonsil removal, a relatively simple operation, is estimated to be like driving 150 miles. When multiplied across the millions of procedures performed worldwide each year, these emissions quickly add up.
Even small, everyday treatments can have surprisingly large environmental impacts. Inhalers, for example, commonly used to treat asthma and other lung conditions, can contain extremely powerful greenhouse gases.
Some of these gases have a global warming potential up to 3,000 times greater than carbon dioxide – a key culprit of climate change. Indeed, inhalers account for over 3% of the total carbon footprint of the National Health Service (NHS) in England alone.
Healthcare emissions are also deeply unequal across the world. Wealthy, technologically advanced countries produce the majority of healthcare related greenhouse gases – with estimates indicating that they account for around 75% of the global total. While poorer countries, which contribute far less to the problem, often face the most severe health consequences of climate change.
Rethinking patient care
But despite the scale of the problem, it is possible to reduce emissions by using different treatments or approaches without compromising patient care.
Where appropriate, this can mean switching patients from high-emission pump inhalers to lower-impact alternatives such as dry powder or capsule-based devices. It could also include doing more procedures as day cases to avoid hospital admissions. Or opting for non-surgical treatment of common conditions instead of operating.
Actually changing clinical practice is, however, a challenge. One of the biggest barriers is that without understanding exactly where emissions occur, it is difficult to identify what changes need to be made and where they’d have the greatest effect.
This is why our team is in the process of measuring the environmental impact of different treatments – from physical training to pain medication, to surgery – to identify the processes responsible for the most emissions.
Although our initial focus will be on a single condition, knee osteoarthritis, our model will eventually be able to be applied more widely across the healthcare system, hopefully allowing real change to occur. This is important because ultimately, hospitals cannot fully protect human health while contributing to the environmental changes that threaten it.
This article was commissioned as part of a partnership between Videnskab.dk and The Conversation, where articles are also published in Danish.























































You must be logged in to post a comment Login